Many people suffer from sensitive teeth for a variety of reasons, this article highlights why you may suddenly develop sensitive teeth, what you can do about it at home, what treatments the dentist may be able to offer you and how to reduce the pain from tooth sensitivity.
What causes tooth sensitivity?
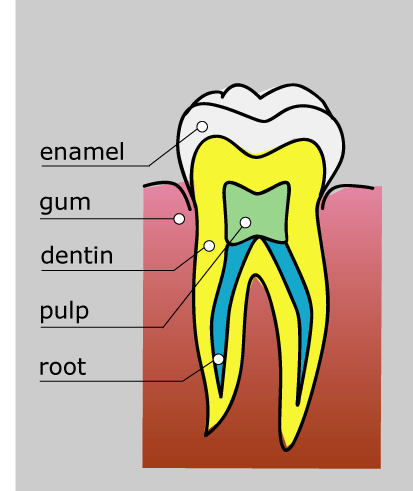 Your teeth are made up of three primary layers:
Your teeth are made up of three primary layers:
- The nerve and pulp. This is the deepest living part of your tooth, it contains the nerve and has blood flowing through it to keep your tooth alive, it is protected by two out of protection layers.
- The dentine. This is the softer portion of your tooth, it gives the tooth it’s primary colour and its role is to support the hard yet brittle outer enamel.
- The enamel. This is the hardest substance in the human body and protects the outer portion of your tooth.
Sensitivity occurs when hot or cold substances, such as eating ice cream, get too close to the nerve, there are many reasons this could happen, including:
- Tooth wear caused by over brushing.
- Gum recession caused by over by over brushing or general ageing.
- Cracked teeth caused by trauma.
- Decay in teeth caused by poor oral hygiene.
- Tooth grinding or clenching.
Why are my teeth suddenly sensitive?
The key to understanding this is to think about how the hot or cold feeling may be getting through to the nerve. If you have had a recent trauma then perhaps the tooth is correct. If you haven’t been to the dentist for a while perhaps there is an area of tooth which is decayed.
The image below shows gum tissue recession around the gum line, possibly caused by over brushing. The enamel is thin in this area which can easily lead to teeth sensitivity.
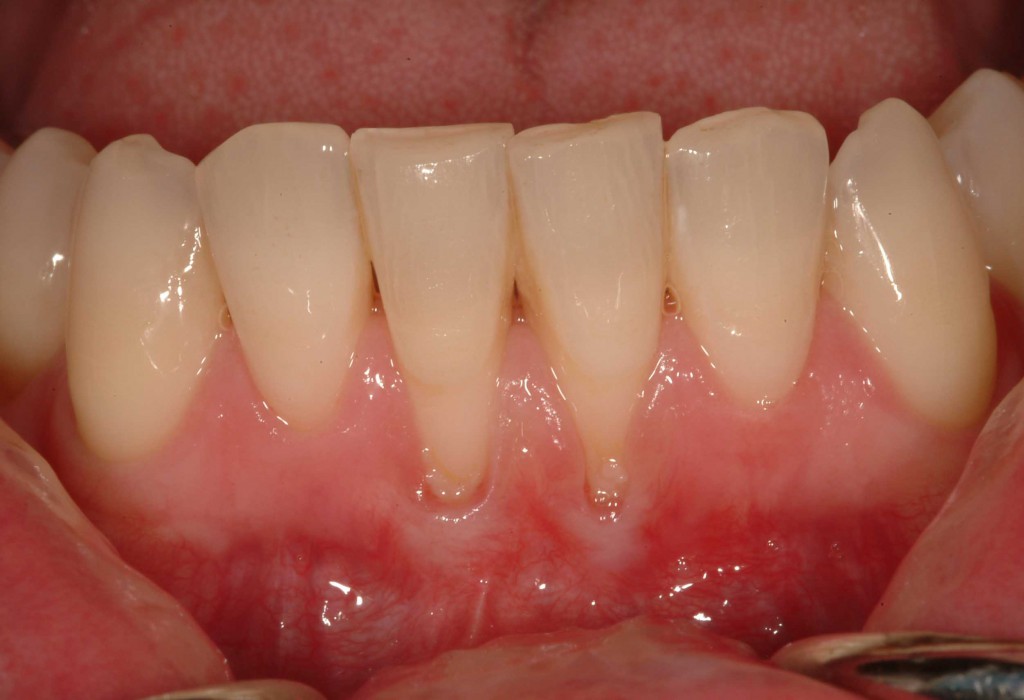
If you can’t immediately identify what the problem is then visiting a dentist or dental hygienist may be best option.
How do you stop sensitive teeth pain
If you have sensitive teeth with no obvious cause then you may find that using a protection and relief toothpaste such as Sensodyne may help.
How does Sensodyne work?
These toothpastes work because there are tiny holes, called tubules, in the dentine of your tooth. If the enamel becomes eroded away then these tubules can transmit the hot and cold through your tooth. These toothpastes work by quickly creating a barrier so that the hot and cold feeling can’t be transmitted to the nerve.
However, it’s worth noting that these types of toothpastes WILL NOT work if the sensitivity is caused by excessive enamel or dentine loss such as cavities, excessive wear or cracks caused by trauma.
How long does tooth sensitivity last?
Tooth sensitivity is usually only instantaneous when the nerve becomes exposed to hot or cold. Remove the hot or cold and the sensitivity goes away. However, the reality is that this is not practical to do on a day by day basis, we have to eat and drink after all! Unfortunately, if your teeth are sensitive they won’t get better on their own, you will either need to use a relief and protection toothpaste or visit a dentist to ascertain why your teeth are sensitive.
What does the dentist do for sensitive teeth?
The basic premise for reducing tooth sensitivity is to protect the outer surface of the tooth to prevent the hot and cold sensations been transmitted through to the nerve, or in extreme circumstances to remove the nerve itself. There are a variety of ways of treating sensitivity at the dentist, including but not limited to:
- Fluoride treatments to strengthen tooth enamel. These fluoride gels can be applied topically at the dentist or trays can be provided for use at home.
- Bonding. Composite bonding materials can be used to bonded to the outer surface of the tooth to rebuild the enamel where it has been lost. This can cover up the dentin hypersensitivity.
- Surgical gum graft (Please see the explanation video below). If the sensitivity is caused by excessive gum resorption which exposes the more sensitive root of the tooth then a gum graft to replacing some of the gum tissue may be undertaken to cover up some of this exposed area around the gum line.
- Root canal. In extreme circumstances a root canal can be used to remove the nerve of the tooth. This is not normally a preferred option and will only be undertaken in extreme circumstances.
Summary
One of the key things to focus on is brushing your teeth and maintaining good dental care throughout your life, ensuring you brush and floss regularly. Tooth sensitivity is a common problem, particularly in later life as the gum becomes more exposed and the teeth wear. Certainly, this is one of the best ways to prevent tooth sensitivity. If you are older then be aware about using a soft bristled toothbrush, watching to ensure you don’t consume too many acidic foods and drinks and be aware if you grind your teeth. Cold air can also affect sensitivity, so you may find you need to wear a scarf in cold weather.


 Gum disease, which includes periodontal disease, is inflammation and infection that destroys the tissues that support the teeth, including the gums, the periodontal ligaments and the tooth sockets (alveolar bone). Gum disease affects more than half of the adult population with natural teeth. It can be treated by a dentist or hygienist and in the early stages the effects can be reversed. There are two main types of gum disease:
Gum disease, which includes periodontal disease, is inflammation and infection that destroys the tissues that support the teeth, including the gums, the periodontal ligaments and the tooth sockets (alveolar bone). Gum disease affects more than half of the adult population with natural teeth. It can be treated by a dentist or hygienist and in the early stages the effects can be reversed. There are two main types of gum disease: